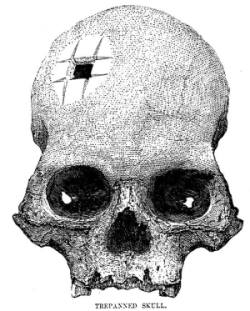
Last week I discussed the history of the medical procedure known as trepanning. This week I will be discussing further the historical elements of the technique as used for both ‘magical’ and also therapeutic purposes, as compared to modern practices.
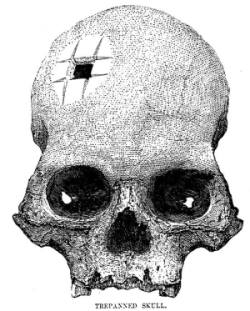 Earliest written references to trepanning exist in the Hippocratic corpus, which suggested that trepannation served as means to release ‘poor humors’, additionally, 13th century texts recommend the opening of the craniums of patients “that the humors and air may go out and evaporate”. Common beliefs at the time attributed ‘bad humors’ to almost every affliction, pain, ache and general concern related to the skull including such mental diseases as epilepsy and depression.
Earliest written references to trepanning exist in the Hippocratic corpus, which suggested that trepannation served as means to release ‘poor humors’, additionally, 13th century texts recommend the opening of the craniums of patients “that the humors and air may go out and evaporate”. Common beliefs at the time attributed ‘bad humors’ to almost every affliction, pain, ache and general concern related to the skull including such mental diseases as epilepsy and depression.
In the Practica Chirurgiae (c.1180), Rogerius of Parma wrote: ‘for mania or melancholy a cruciate incision is made in the top of the head and cranium penetrated to permit the noxious material to exhale to the outside.’ This appears to derive from Greek medicinal belief that stagnant blood, much like stagnant air, should be released and allowed to flow freely, but also that blood itself contained elements integral to mental health, such as depression or melancholy.
There is little historical evidence supporting current claims as to the efficacy of ‘voluntary trepannation’, by which it is claimed that drilling of the skull increases cognitive capacity and creativity. It appears our forefathers knew better. I for one am with the critics of voluntary trepannation, but the same critics protesteth too much; I do not feel our society has much to lack from the loss of idiots who seek to improve cognitive function by drilling into their skulls, as for someone to hold such a personal belief their intelligence had nowhere to go but up, and inevitable failure of their efforts might leave the world a few fools lighter. But this is merely my opinion.
In any case, historically compression or depression of the bone alone was not a prerequisite for trepannation, caused by either trauma or impact relating to falls, although throughout history it was considered prudent to remove fractured sections of the skull to prevent further damage or piercing of the brain itself. Greek methods employed the use of a bow or drill rolled between the palms, with water to diminish heat generated from the friction.
 Most trepannation techniques performed in Saharan cultures as well as Incan and Mayan, whether or not citing a spiritual bases for procedure, sought to reduce pressure in the cranial cavity by means of drilling, yet seek to simultaneously remove “evil spirits, … vapors, humors, pressures and imagined foreign bodies in the head. In historical accounts of claimed ‘daemonic possession’, little is considered out-of-bounds, and skull-boring was used to allow passage of the evil spirits from the body.
Most trepannation techniques performed in Saharan cultures as well as Incan and Mayan, whether or not citing a spiritual bases for procedure, sought to reduce pressure in the cranial cavity by means of drilling, yet seek to simultaneously remove “evil spirits, … vapors, humors, pressures and imagined foreign bodies in the head. In historical accounts of claimed ‘daemonic possession’, little is considered out-of-bounds, and skull-boring was used to allow passage of the evil spirits from the body.
It is quite simple to translate the term ‘evil spirits’ as an early interpretation of the now more nuanced and multifaceted view of the both cranial physiology as well as the human mental condition. It also bears reiterating the survival rate of so-called primitive societies performing the procedure, compared to the now almost lethal application of such a surgery (I believe that my successful procedures are the only things holding up an already deplorable western average). It is due only to the utter incompetence of contemporary physicians and the despicable conditions of hospitals that the modern practice of trepannation is considered a dangerous procedure at all.
In 1865 our mortality rate for an average hospital stay stood at little over 30%. We are supposedly in an age of discovery, yet dissenting minds lambast trepanning whilst condoning such crack-pot sciences as blood-letting (last year almost 41 million leeches were imported from France alone). Consider the moron Sir Astley Cooper who stated ‘…if you were to trephine, you ought to be trephined in turn’. Some do not seek to risk their already spotty reputations by accepting that for a number of ailments (when the correct techniques are applied) trepanning can remain a major force in the recovery of patients.
(This article was originally posted in The Pandora Society on December 24 2014)